קמגרה ישראל
היבואן הרשמי
קמגרה®: פתרון יעיל, בטוח, ומהיר!
- כל תכשירי הזקפה באתר הינם 100% מקוריים
- כך תזהו קמגרה מקורית
היבואן הרשמי



2 שקיות קמגרה ג'ל במתנה בכל קנייה מעל 379 ₪ עם הקופון: GET2

קמגרה ישראל פועלת ישירות מול יצרנית הקמגרה Ajanta Pharma – חברה בינ”ל מוערכת עם אישורי FDA.
הזמנת קמגרה דרך קמגרה ישראל (היבואן הרשמי) מבטיחה קבלת קמגרה 100% מקורית.
רכישה של קמגרה ניתן לבצע דרך האתר / וואצאפ / או בטלפון 053-7624465 ולקבל משלוח מהיר. אנו מציעים משלוחים בכל רחבי ישראל במחיר משתלם. אנו מתחייבים לספק את המוצר המקורי ב 100 האחוזים – באחריות! אם חיפשת קמגרה ג’ל [Kamagra Oral Jelly] להעצמת החוויה שלך, במגוון טעמים, תוכל כעת לקבל את המוצר בדיסקרטיות מלאה עם משלוח מהיר בכל עיר בשטחי ישראל.
ישראל היא מדינה שנמכרים בה תחליפי ויאגרה רבים ולצערנו התחום לא מספיק מפוקח. סוחרים רבים החלו לייבא תחליפים וחיקויי קמגרה מהמזרח הרחוק בזכות הזמינות הגבוהה של תכשירים אלו ומחיריהם הנמוכים. זוהי תופעה שאנו מזהירים מפניה ואף נלחמים בה. אצלנו, קמגרה ישראל היבואן הרשמי – תקינותו של כל תכשיר נבדקת ונבחנת היטב. התכשירים הנמכרים הינם תכשירים מקוריים ברמה הגבוהה ביותר. חשוב לפני השימוש לבדוק בקפדנות את ההוראות ולהתייעץ עם רופא, במיוחד אם ידועה רגישות ו/או אם הנכם נוטלים תרופות כלשהן.
קמגרה ישראל מביאה אליכם מגוון מוצרים ייחודיים ומקוריים – תחליפי ויאגרה במחיר נוח. כיום, ישנם רבים שמתקשים להשיג טיפול בבעיות מין בשל המחירים הגבוהים של מוצרי הטיפול הרגילים. כעת תוכלו לקבל טיפול איכותי שיסייע לכם לשפר את הביצועים במיטה ואת איכות החיים כולה – וכל זה במחיר נוח ותחרותי. המחירים שלנו הינם הכי טובים למוצר המקורי. אנו גאים בהנגשה של תכשירי זקפה לקהל גדול של גברים המעוניינים בפתרונות אמיתיים. אנו כאן על מנת לספק לכם שירות מקצועי ומסור ברמה הגבוהה ביותר.


קמגרה GOLD – חזקה ואפקטיבית במיוחד בשיפור הזקפה
מוצר איכותי מבית קמגרה ישראל במחירים הכי טובים שתמצאו בישראל. התכשיר מסופק במשלוח דיסקרטי ומהיר.
לידיעתכם, אנו מוכרים אך ורק מוצרים מקוריים.
קמגרה היא תכשיר פרמצבטי לטיפול בבעיות זקפה. היא ידועה ביעילותה ובמהירות פעולתה, וניתן לרכוש אותה ללא מרשם רופא.
קמגרה מסייעת בזרימת הדם לאזור הפין, וכך משפרת את הזקפה ומחזקת אותה. היא גם עשויה להגביר את החשק המיני.
החומר הפעיל בקמגרה הוא סילדנפיל. סילדנפיל פועל על ידי הרחבת כלי הדם באזור הפין, וכך מאפשר זרימה טובה יותר של דם.

מה חשוב לדעת?
לסיכום:
קמגרה היא תכשיר פרמצבטי יעיל ובטוח לטיפול בבעיות זקפה. היא זמינה ללא מרשם רופא וניתן לרכוש אותה בקלות.
עקרון הפעולה של קמגרה (Kamagra) מבוסס על הפטנט של ויאגרה, אבל ניתן גם להכתיר את קמגרה בתור היורשת החוקית של ויאגרה וזאת בזכות רשימה ארוכה ומכובדת של יתרונות כגון: אפשרות לשימוש מיידי! (דקות ספורות עד שהסילדנאפיל, החומר הפעיל, נכנס למחזור הדם) • נוחות שימוש מירבית במיוחד כאשר צורכים את התכשיר בצורת סוכריות או ג’ל • הכי מעט תופעות לוואי ביחס לתכשירים אחרים • ועוד יתרונות כולל מחיר נוח יותר בכיס!
כשמכירים את יתרונותיה של קמגרה אין סיבה להביט לאחור – נסו ולא תתחרטו! מדובר במוצר הכי נמכר ב 2024 לשיפור התפקוד המיני בישראל. אלפי גברים כבר התמכרו להנאה שתכשירי קמגרה מאפשרים במיטה. הנאה שמשפרת גם את הרומנטיקה וגם את הזוגיות (עם קמגרה, גם אם אתם עדיין לא בזוגיות, הרבה בנות ירצו את מה שיש לכם להציע במיטה).
באמצעות האתר ניתן למצוא את המוצרים הנדרשים ולהוסיף אותם לסל הקניות שלכם. כל התשלומים מתבצעים בצורה מאובטחת לחלוטין. תשכחו מכל מה שלמדתם על קניות אונליין. אנו מקבלים מגוון רחב של אמצעי תשלום. באפשרותכם לשלם במזומן אם כך נוח לכם.
כמו כן, האתר מאפשר לכם להזמין קמגרה בצורה אנונימית, אם אינכם רוצים להיחשף. גם המשלוחים מתבצעים באופן דיסקרטי לחלוטין ללא שאילת שאלות ובמהירות האפשרית, כך שתוכלו לקבל את המוצרים שלכם בצורה מהירה, נוחה ובטוחה.
קמגרה ישראל האתר הרשמי מציע חווית קניות מהירה, מאובטחת ונוחה עם אפשרות לקבלת שירותים ומבצעים מיוחדים.
אנו מציעים אפשרויות רבות לרכישת מוצרי קמגרה בקלות ובנוחות. תוכלו לבחור את צורת ההזמנה המועדפת עליכם: דרך וואצאפ, בטלפון או באמצעות סל הקניות באתר. קמגרה ישראל הוא אתר אינטרנט מוביל בתחומו, בעל שכבות אבטחה רבות. אנו מציעים משלוחים מהירים בערי ישראל השונות ותוכלו גם לקבל הנחות על קנייה גדולה. קמגרה ישראל מחזיקה מלאי תכשירים מקוריים רחב – הזמין לרכישה מכל מקום בישראל.
עבורנו הלקוח הוא מעל הכל, ולכן אנו מספקים שירות לקוחות אדיב ומקצועי במגוון ערוצים, כגון מייל, וואצאפ וטלפון. אנו מבטיחים לטפל בכל בקשה שלכם במהירות ובמקצועיות, ולהשיב לכל שאלה בצורה מסודרת וברורה. אם יש לכם שאלות או בקשות, אל תהססו ליצור איתנו קשר דרך הערוצים הנ”ל ונשתמע בקרוב!
סקרנים לגבי זמן השפעה של קמגרה ג’ל? התכשיר נכנס לפעולה זמן קצר לאחר בליעתו (תוך 10 ל-30 דקות) והשפעתו נמשכת בין 4 ל-6 שעות.
בכל מקרה כדי ליהנות מהרגע המושלם עם בת זוגכם אין לצרוך יותר מהמינון המקסימלי שהינו שקית אחת ליום.
גברים רבים בוחרים בתכשירי קמגרה לקבלת ההשפעות הידועות של Viagra בתוספת כמה יתרונות – כגון ספיגה מהירה, נוחות השימוש, ועוד. בדומה לתכשירים נוספים לשיפור התפקוד המיני, קמגרה מהווה תחליף ויאגרה והוא מבוסס על אותו חומר פעיל כמו בוויאגרה, ולכן מכונה לעיתים “ויאגרה גנרית”.
השימוש בתכשירי קמגרה יכול להועיל לגברים רבים משום שמדובר בתכשיר המיועד להגברת החשק המיני וההנאה מיחסי המין. קמגרה מיועדת לגברים המעוניינים להגיע לזקפה מלאה וממושכת יותר – בין אם הם מתקשים להגיע לזקפה מלאה, ובין אם ברצונם להאריך את משך הזקפה. בכל המקרים התוצאה זהה: שיפור יחסי המין וכתוצאה מכך שיפור הזוגיות ואיכות החיים.
קמגרה מאפשרת לך להיות מוכן לפעילות מינית מתי שתחפוץ ובאופן מיידי. ג’ל קמגרה ניתן לקחת רבע שעה בלבד לפני האקט המיני.
ברגע שתחוש גירוי מיני, קמגרה תיכנס לפעולה, ותחווה זיקפה מחוזקת אשר מעצימה את יכולותיך במיטה.
קמגרה מותרת לצריכה אישית. אין מניעה חוקית לצרוך קמגרה מהטעם שמדובר בתוסף תזונה מכל בחינה רלוונטית לרכישה ולשימוש אישי בקמגרה.
אין הרבה נתונים בנושא אך לפי מחקר שנערך בנושא בסקוטנלד, מומלץ להימנע משילוב של קמגרה עם קנאביס משום שהדבר עלול להוביל לעלייה בסיכון לאירוע לבבי. לפי מחקר אחר שנערך בקנדה, קנאביס משפיע לרעה על הזקפה ובכלל על תפקוד מערכת הרבייה הגברית, כך שבאופן כללי לא מומלץ להפריז בצריכת קנאביס.
כדי להבטיח יעילות מקסימלית, עליכם לעקוב אחר הוראות השימוש בתכשיר ובכלל זה יש לצרוך את הג’ל על קיבה ריקה, לא לצרוך אלכוהול, ולהמתין כ-15 דקות לפני האקט המיני. שימו לב שצריכת התכשיר על קיבה מלאה עלול פשוט להוביל לעייפות משמעותית מה שלא תורם לאקט המיני.
קמגרה עוזרת ליצירת זקפה מחוזקת לאחר כ 15 דקות מרגע נטילת התרופה. אך אל דאגה, ההשפעה של קמגרה תלויה בגירוי מיני, כך שברוב המקרים תרגישו אותה רק בזמן קיום יחסי מין. התכשיר כשלעצמו, ללא גירוי מיני, אינו גורם לזקפה. כך שתוכלו להמשיך בשגרת יומכם ללא כל חשש, וללכת לכל מקום גם אם לקחתם קמגרה ב 6 השעות האחרונות.
עם קמגרה אתם יכולים לתכנן את הערב שלכם בכיף גדול, לצרוך את התכשיר כרבע שעה לפני האקט ולדעת שהלילה הקרוב עומד להיות סוער ומהנה. השפעת הקמגרה נמשכת בין 4 ל-6 שעות – וכן, התכשיר בהחלט עשוי לעזור לכם להגיע ליותר אורגזמות ולהחזיק יותר זמן.
קמגרה לכשעצמה אינה ממכרת. תוכלו לצרוך את התכשיר רק מתי שאתם בוחרים ורוצים לקבל בוסט ליכולת ולכושר המיני שלכם או כאשר אתם נערכים ללילה סוער ורוצים להחזיק יותר זמן מהרגיל.
לא ידוע על הפחתה ביעילות בשימוש מתמשך. כל עוד לא עוברים על המינון המומלץ (שקית קמגרה ג’ל ביום) לא אמורה להיות בעיה.
התכשיר מחזק את האון הגברי וגורם לזקפה חזקה, ביצועים משופרים, גירוי מיני מוגבר – כך שהתוצאה היא העצמת הסיפוק וההנאה עבור שני הצדדים.
אלכוהול – שתיית אלכוהול עלולה בחלק מהמקרים להוביל לסחרחורת ותחושת טשטוש קל וכך גם תרופות לחיזוק זקפה כגון קמגרה. שילוב של שני חומרים אלו עלול להוביל לסחרחורת ואף להתעלפות. כמו כן, שילוב זה עלול להוביל לכאבי ראש או מיגרנה, במיוחד עבור מי שסובל מכאבי ראש לעיתים קרובות.
כמו לכל תכשיר רפואי הנצרך דרך מערכת העיכול, גם לקגמרה עשויות להיות תופעות לוואי (שאינן חמורות או מסוכנות), המצוינות על גבי האריזה. אם ידועה לכם רגישות לתרופות, כדאי להכיר מראש את התסמינים שעשויים להופיע. תופעות הלוואי שעלולות במקרים נדירים להופיע כוללות כאב ראש, בחילה, אדמומיות או גודש באף ובדרכי הנשימה העליונות, כאבי בטן ואפילו במקרים חמורים יותר – קלקול קיבה.
אין להשתמש בקמגרה במקביל לטיפול תרופתי ביתר לחץ דם. השימוש בקמגרה אסור למקבלים תרופות ממשפחת הניטרטים כמו מונוניט, איזוקט, מונוקורד ומונולונג. אין להשתמש בקמגרה אם אתה סובל מבעיות לחץ דם, תפקודי כבד, ותפקודי לב או כליות. השימוש אסור גם לאלרגים לסילנדפיל. אם הופיעו תופעות לוואי כלשהן המוזכרות לעיל, יש להפסיק מיידית את השימוש בתכשיר.
הפתרון שחיפשת, שחלמת להשיג, אולי במשך שנים רבות- קמגרה! אנחנו, קמגרה ישראל כאן כדי לעזור לגברים ממש כמוך להתגבר על הקשיים בתחום המיני, כי אנחנו יודעים כמה זה חשוב לך וכמה שזה משפיע על כל תחומי החיים. אחרי שראינו שוב ושוב את ההשפעה המדהימה של קמגרה על גברים רבים, אפשר כבר לדבר במונחים של שליחות.
המוצר הנמכר ביותר באתר הוא קמגרה ג’ל [kamagra oral jelly] שכשמו כן הוא – ג’ל המזכיר את תוסף המזון שספורטאים משתמשים בו כדי להשיג תוצאות טובות יותר בענפי הספורט השונים – וגם במקרה שלנו, קמגרה ג’ל מספק שיפור מורגש מאוד בביצועים. אפשרות פופולרית נוספת היא קמגרה גולד [kamagra gold] – תכשיר בעוצמה כפולה ומחיר אטרקטיבי.
כדי להקל עליך אנו מאפשרים הזמנת מוצרי קמגרה ללא מרשם רופא כך שתוכל להתחיל באופן מיידי את השימוש בג’ל.
חיכית די והותר לרגע הזה, נכון?
יש לך שאלה?
לחץ, חרדה, גורמים פיזיים כאלה ואחרים – כולם תורמים לירידה בכושר המיני. ובמדינה כמו ישראל כמובן שיש לא מעט גורמי לחץ. במקרים מסוימים זה כמעט בלתי מורגש, אך עבור חלק מהגברים זאת בעיה של ממש בין אם מדובר על שפיכה מוקדמת או על אין אונות.
זה מסוג הדברים שמעיבים על תחושת המסוגלות שלך כגבר ולא פעם גם מכרסמים בביטחון העצמי. גברים שמוצאים את עצמם בסיטואציה כזאת באמצע החיים פתאום נדרשים להתמודד עם בדיקות רפואיות, התייעצות עם רופאים ולעיתים גם התערבות ניתוחית. הבעיה כאן היא קודם כל מידת החשיפה האישית שלא כולנו מוכנים לה – ושנית כל, לו רק ניתן היה לחסוך את כל הביורוקרטיה ולקצר תהליכים מורכבים…
לפעמים כל מה שצריך זה פתרון נקודתי שיספק הקלה ויחזיר את האוויר לריאות ואת הסומק ללחיים. קמגרה עושה את זה. היא משפרת את רמת התפקוד המיני. במילים אחרות, הזקפה שלך תפתיע אותך כי פתאום יהיה לך הרבה יותר קל להגיע לזקפה מלאה שנשארת לאורך זמן. קהל היעד של תכשירי קמגרה הינו רחב למדי – אם אתה סובל מבעיות בתפקוד המיני, תגלה כי קמגרה מאפשרת לך לתפקד בצורה נורמלית כאילו הבעיה לא קיימת כלל! ואם אין לך בעיה תפקודית מיוחדת – הקמגרה תוכל לתת לך בוסט מטורף ולאפשר לך להגדיל את ההנאה מהפעילות המינית, שזה אומר יותר זמן שתצליח להחזיק, ויותר פעמים שתוכל לגמור.
אם ויאגרה סיאליס ודומיהם מצריכים ממך לצאת ל”טיול” בין רופאים ובתי מרקחת – קמגרה חוסכת לך את הכאב ראש. לא קיים מושג של “ללכת לקנות קמגרה” – פתרנו את זה עבורך: קמגרה מגיעה אליך. ההבדל הזה משנה את כל חווית השימוש בתכשירי קמגרה.
החלטת לתת צ’אנס לתכשירי קמגרה? גם כאן אתה לא לבד. מיליוני גברים מסביב לעולם וגם ברחבי ישראל עושים שימוש יומיומי בתכשירי קמגרה מכיוון שהם משדרגים להם את ההנאה מחיי המין. ומכיוון שזה דבר כל כך נפלא, הבשורה מכה גלים וכך זכתה קמגרה בפופולריות העצומה שיש לה כיום.
אבל אל תסמוך רק על המילה שלנו. אין דבר יותר קל מאשר להזמין אריזה של תכשיר קמגרה מקורי ופשוט להתנסות בעצמך ולראות אם כל התשבוחות ששמעת על מוצרי קמגרה אכן מוצדקות. הודות לרמת הדיסקרטיות הגבוהה שאנו מציעים, לצד שירות משלוחים בפריסה מלאה (בתוך הקו הירוק של ישראל). מעולם לא היה קל יותר לרכוש מוצר כל-כך אפקטיבי ומדהים לשיפור התפקוד המיני.
מהלקוחות הרבים שלנו אנו שומעים רק דברים טובים לגבי קמגרה. רובם המוחלט של הלקוחות מזמינים שוב ושוב – כי המוצר עובד וכתוצאה מזה לא רק שהביטחון העצמי משתפר אלא שאותם גברים נראים יותר ויותר קורנים, הבריאות הכללית שלהם משתפרת, הזוגיות שלהם משתפרת כך ש…
צוות קמגרה ישראל ליקט את השאלות הנפוצות ביותר. כל המידע לפניכם:
גברים רבים בוחרים בתכשירי קמגרה לקבלת ההשפעות הידועות של הוויאגרה בתוספת כמה יתרונות (השפעה מהירה, קלות השימוש, ועוד). בדומה לתכשירים נוספים לשיפור התפקוד המיני, קמגרה מהווה תחליף ויאגרה והוא מבוסס על אותו חומר פעיל כמו בוויאגרה (ולכן מכונה לעיתים “ויאגרה גנרית”).
גברים רבים יכולים להפיק ערך רב מתכשירי קמגרה, שכן מדובר בתכשירים המסייעים להגברת החשק המיני וההנאה ממגע מיני. ליתר דיוק, קמגרה מיועדת לשימוש על ידי גברים המעוניינים להגיע לזקפה מלאה וארוכה יותר – בין אם הם מתקשים להגיע לזקפה מלאה, ובין אם הם רוצים להאריך את משך הזקפה. בכל המקרים התוצאה זהה: שיפור המין וכתוצאה מכך שיפור מערכות היחסים ואיכות החיים.
קמגרה ג’ל (kamagra oral jelly) הינו ג’ל בטעמי פירות על בסיס גליצרין צמחי ובתוספת החומר הפעיל הקיים בכדורי ויאגרה. ג’ל קמגרה נספג במהירות וגורם לזקפה מלאה וממושכת. קמגרה ג’ל מתאים לגברים שלא מתחברים לבליעת כדורים ורוצים לשפר את התפקוד המיני ובכך להגביר את ההנאה.
צריכת קמגרה מאפשרת לכם להיות מוכנים לפעילות המינית בשיא המהירות. את הג’ל ניתן לקחת רבע שעה בלבד לפני האקט המיני. ברגע שתחושו גירוי מיני, קמגרה תיכנס לפעולה, ותחושו בזיקפה מחוזקת אשר מעצימה את יכולותיכם.
קמגרה מחזקת את האון הגברי וגורמת לזקפה חזקה, ביצועים משופרים, גירוי מיני מוגבר – כך שהתוצאה של שימוש בתכשירי קמגרה היא העצמת הסיפוק וההנאה עבור שני הצדדים.
קמגרה לכשעצמה אינה ממכרת. תוכלו לצרוך Kamagra רק מתי שאתם בוחרים ורוצים לקבל בוסט ליכולת ולכושר המיני שלכם או כאשר אתם נערכים ללילה סוער ורוצים להחזיק יותר זמן מהרגיל.
קמגרה נכנסת לפעולה זמן קצר לאחר בליעתה (תוך 10 ל-30 דקות) והשפעתה נמשכת בין 4 ל-6 שעות. כדי ליהנות מהרגע המושלם עם בת זוגכם, אין לצרוך יותר מהמינון המקסימלי שהינו שקית קמגרה אחת ליום.
קמגרה עוזרת ליצירת זקפה מחוזקת לאחר כ 15 דקות מרגע נטילת התרופה. אך אל דאגה, ההשפעה של קמגרה תלויה בגירוי מיני, כך שברוב המקרים תרגישו אותה רק בזמן קיום יחסי מין. התכשיר כשלעצמו, ללא גירוי מיני, אינו גורם לזקפה. כך שתוכלו להמשיך בשגרת יומכם ללא כל חשש, וללכת לכל מקום גם אם לקחתם קמגרה ב 6 השעות האחרונות.
אף פעם לא מוקדם מדי להתחיל לתכנן לילה נהדר. קח קמגרה 15 דקות לפני האקט ותיהנה מהלילה של חייך – כשעוד שעות רבות נותרו לפעילויות אחרות, כמובן. ההשפעה של קמגרה תורגש במשך 4-6 שעות, אז קדימה, תכננו את הערב שלכם!
קמגרה ג’ל מכילה חומר פעיל כמו בוויאגרה סילדנפיל. הג’ל מכיל רכיבים נוספים כגון גליצרין צמחי שהוא חומר נפוץ בתעשיית התרופות. מה שמקנה לג’ל את טעמי הפירות הם חומרי טעם וריח בדומה למה שקיים בסוכריות וממתקים.
ניתן להשיג קמגרה ללא מרשם. היוצאים מהכלל הינם גברים המטופלים בתרופות כלשהן על בסיס קבוע – ובמיוחד תרופות להסדרת זרימת הדם. במקרים אלו חובה להיוועץ עם רופא טרם השימוש בתכשיר.
השימוש בתכשירי קמגרה הינו בטוח לחלוטין אך בכדי למנוע סיכון מיותר, על כל אדם שצורך תרופות על בסיס קבוע להתייעץ עם הרופא שלו, וזאת כדי לוודא שהתרופה שהוא נוטל בטוחה לשימוש במקביל לשימוש בתכשיר הקמגרה.
לסיכום, הזמנת קמגרה אינה מצריכה מרשם או בדיקות רפואיות, ולכן ניתן להזמין משלוח עד הבית בנוחות מרבית ודיסקרטיות מלאה.
כדי להבטיח יעילות מקסימלית, עליכם לעקוב אחר הוראות השימוש בתכשיר ובכלל זה יש לצרוך את הג’ל על קיבה ריקה, לא לצרוך אלכוהול, ולהמתין כ-15 דקות לפני האקט המיני.
קמגרה ג’ל הוא תחליף ויאגרה שנחשב ליעיל. רוב המשתמשים בתכשיר מעידים עליו שהוא בטוח לשימוש ובעל מספר מועט מאוד של תופעות לוואי (אם בכלל). יחד עם זאת,
כמו לכל תכשיר רפואי הנצרך דרך מערכת העיכול, גם לקגמרה עשויות להיות תופעות לוואי (שאינן חמורות או מסוכנות), המצוינות על גבי האריזה.
כדאי להכיר מראש את התסמינים שעשויים להופיע, במיוחד אם ידועה לכם רגישות לתרופות. הכנה מוקדמת מאפשרת היערכות טובה יותר ונקיטה בגישה זהירה יותר בטרם מתחילים לצרוך את התכשיר. כמו כן, כאשר מבינים אילו סייגים והתוויות קיימים לשימוש בתכשיר, אפשר להשתמש בו בצורה נכונה, נוחה, ובטוחה יותר.
תופעות הלוואי שעלולות במקרים נדירים להופיע כוללות כאב ראש או בחילה, אדמומיות או גודש באף ובדרכי הנשימה העליונות, כאבי בטן ואפילו במקרים חמורים יותר – קלקול קיבה.
קמגרה אסורה לשימוש לאנשים שמשתמשים בתרופות מרחיבות כלי דם ממשפחת הניטרטים, כגון מונוניט, מונוקורד.
אלכוהול
שתיית אלכוהול עלולה בחלק מהמקרים להוביל לסחרחורת ותחושת טשטוש קל וכך גם תרופות לחיזוק זקפה כגון הקמגרה. שילוב של שני חומרים אלו עלול להוביל לסחרחורת ואף להתעלפות. כמו כן, שילוב זה עלול להוביל לכאבי ראש או מיגרנה, במיוחד עבור מי שסובל מכאבי ראש לעיתים קרובות.
תכשירים נוספים לשיפור התפקוד המיני
קמגרה לא זקוקה לשום חיזוק נוסף. זהו פתרון מלא לשיפור התפקוד המיני. צריכה של קמגרה יחד עם תרופות אחרות או אפילו תכשירים טבעיים לשיפור האון – ברוב המקרים שילוב זה גורם להשפעה מוגברת ולתופעות לוואי משמעותיות. בייחוד יש לשים לב למוצרים שמשפיעים על זרימת הדם. צריכה שלהם יחד עם ג’ל קמגרה מעלה את הסיכון לפתח זקפה ממושכת וכואבת המצריכה טיפול רפואי.
מיץ אשכוליות ומיץ רימונים
מיץ אשכוליות ומיץ רימונים – יחד עם קמגרה הם עלולים לגרום לתופעות לוואי קשות ולעתים אף מסוכנות, כולל כאבי ראש, קשיי עיכול, הסמקה, הפרעות ראייה והפרעה בקצב הלב. מיצים אלה מעלים את רמת התרופה בדם ולכן רצוי להימנע מהם כל עוד אתם בהשפעת הקמגרה.
בנוסף – ברוב המקרים, קמגרה מתחילה לפעול אחרי 10 דקות עד חצי שעה, אך אם תצרכו את התכשיר עם מיץ אשכוליות, הוא יפעל באיחור, מה שמגביר את הסיכון לתופעות לוואי קשות (וכמובן גם לאכזבה).
צמחי מרפא המשפיעים על הלב
חילבה, לוען, ציפורני השטן, עוזרד, דבקון לבן, ילקוט הרועים, זנב הארי ואצבעונית ארגמנית (דיגיטליס)
מכיוון שתרופות לחיזוק הזקפה מגבירות את הסיכון לתופעות לוואי הקשורות ללב וכלי הדם, השילוב עם הצמחים הנ”ל עלול להיות מסוכן ולכן לא מומלץ לצרוך תוספים צמחיים שיגבירו את הסיכון לבעיות אלו.
לא ידוע על ירידה ביעילות בשימוש מתמשך. כל עוד לא עוברים על המינון המקסימלי (שקית/כדור קמגרה ביום) לא אמורה להיות בעיה.
רכישת תכשיר מזויף עלולה להיות מסוכנת לבריאותכם. לא תדעו בהתחלה שזה זיוף כי זיופים המגיעים מטורקיה, סין או תאילנד מכילים גם סילדנפיל ציטראט. הבעיה היא שתכשיר שנוצר בצורה לא מבוקרת משמעותו מינונים לא ידועים וטריות המוצר מוטלת בספק. כמובן שגם רשימת הרכיבים עשויה להשתנות ולא בהכרח לטובה. התוצאה עלולה להיות לילה בבית חולים. כדי למנוע אי נעימות ומבוכה גדולה ריכשו רק מהיבואן הרשמי, רק מקמגרה ישראל בכתובת קמגרה.com.
הקפידו לקנות מאתר היבואן הרשמי – קמגרה.com
השאר פרטים ונחזור אליך במהירות
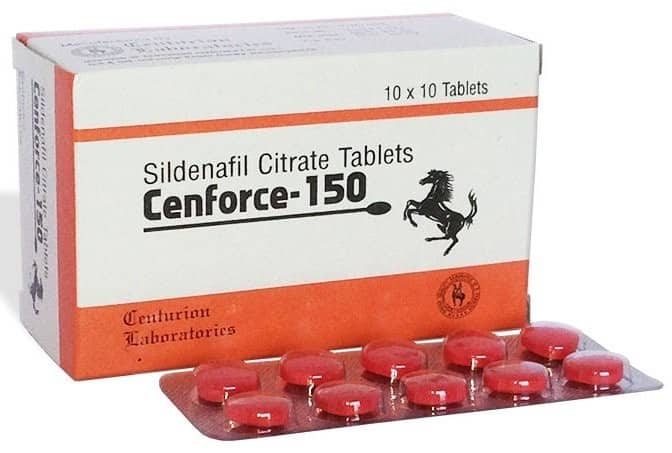
מוצר מוצלח נוסף מבית קמגרה ישראל:
ויאגרה גנרית עם החומר הפעיל sildenafil – בדיוק כמו בוויאגרה. התכשיר עוזר להגיע לזקפה מלאה וארוכה ומאפשר חוויה מינית מענגת ומלאה. מינון: כדור אחד כחצי שעה עד שעה לפני האקט [ההשפעה נמשכת עד 8 שעות].
אסור להעתיק, לצלם, לשכפל, להדפיס או לעשות כל שימוש אחר למטרות מסחר במבנה, תכני, גרפיקה, תמונות ועיצוב האתר ללא אישור מפורש מראש ובכתב מחברת קמגרה ישראל.
